
Lifestyle medicine assessment in veteran care – clinical fact sheet and MCQ
Overview
Lifestyle medicine provides the opportunity to addresses the behavioural, social and environmental factors that underpin many chronic conditions common in Australian veterans, including cardiometabolic disease, chronic pain, mental health conditions, and sleep disturbance.
The pillars of lifestyle medicine include:
- physical activity
- nutrition
- sleep
- stress management
- social connection
- smoking cessation and alcohol harm reduction
For veterans, these lifestyle factors can be strongly shaped by service-related routines, physical conditioning, team identity, and the disruption that often follows transition from Defence. Importantly, these factors interact: poor sleep exacerbates pain and mood disturbance; social isolation increases alcohol use; and physical inactivity accelerates metabolic risk.
Effective care therefore requires deliberate, structured assessment of these factors and what is influencing them in that individual, even when only one or two are addressed initially.
Performing a holistic lifestyle assessment
A holistic lifestyle assessment extends beyond standard risk factor screening. Tools such as the Veteran Health Check and the VETERANS Lens support structured review of:
- service history and transition experience
- trauma exposure
- loss of routine or identity
- current social supports
This approach recognises that many health behaviours are adaptive responses to service demands and transition stressors, rather than simple ‘poor choices’.
During assessment, identify:
- priority lifestyle domains linked to current health concerns
- functional limitations, such as pain, fatigue, or sleep disruption
- veteran-defined goals and values
- current supports and barriers to change
Brief tools can streamline this process. The Lifestyle Medicine Vital Signs tool, developed by the Australian Society of Lifestyle Medicine, provides a rapid, patient-completed overview of key lifestyle domains and can integrate into routine general practice workflows.
Assessing readiness for change
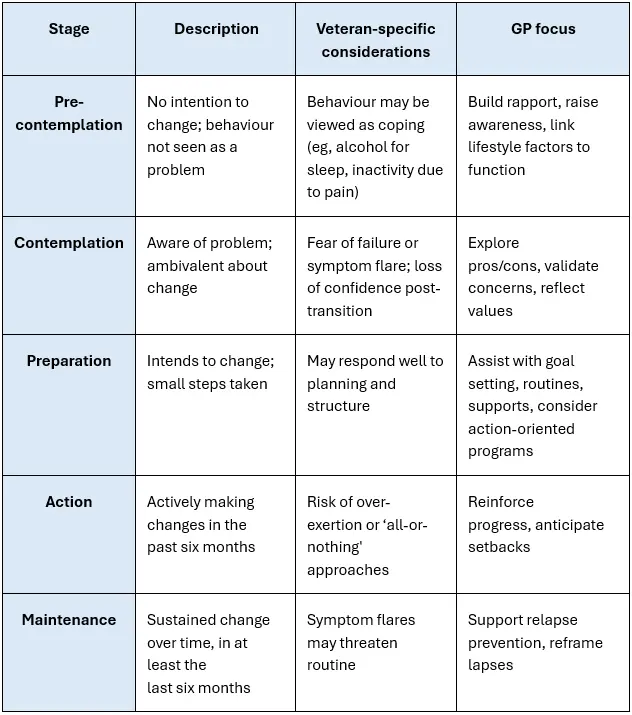
After the initial lifestyle assessment, assessing readiness for change can help formation of veteran-driven goals. The transtheoretical model of change (TTM) provides a practical framework for tailoring lifestyle discussions to an individual’s readiness for change.
People may not be consistent across different domains. For example, they may be prepared to address sleep but pre-contemplative about alcohol use. Recognising the stage of change helps avoid mismatched interventions and supports more effective, trauma-informed engagement motivational interviewing, which may help the person to shift closer to change if they are not ready in that area. A unique factor that may impact the flow of care is the DVA claims process. The process of submitting claims, and claim status, can impact access to care and may influence veteran’s readiness for change.
Identifying motivators in veterans
Veterans commonly identify loss of camaraderie, routine, and identity as major challenges following separation from service. The following levers may enhance engagement with lifestyle discussions:
- team-based framing: positioning healthcare as a new veteran-centred team, including the GP, other healthcare professionals, and the veteran's family members
- performance and capability mindset: focusing on rebuilding function rather than correcting deficits
- routine and structure: encouraging consistent daily patterns to restore control and purpose
- choice and consent: offering options (eg, group vs individual programs) to support autonomy and confidentiality
- gradual progression: starting with achievable goals and building on success
- self-agency: actively involving veterans in planning and decision-making and identification of what will work for them
- acknowledgement of service: recognising service experience to build trust and rapport
What can be done in a brief consult
Even short, dedicated GP consultations can initiate effective lifestyle medicine. If the consult on the day does not present adequate time, then asking the veteran to book another focussed appointment would enable further discussion on a chosen domain. It can help to begin with the patient’s perspective by asking which aspects of lifestyle they feel could be improved and then exploring those areas in more depth.
In a brief consult, GPs can:
- ask permission to discuss lifestyle factors
- identify one priority domain
- undertake basic measurements where appropriate (eg, weight, waist circumference)
- provide brief written information or tools
- suggest allied health input
- schedule a follow-up appointment to discuss a domain in depth
A client-centred counselling style that promotes self-management is particularly important for veterans, supporting autonomy while identifying and leveraging existing skills, discipline, and resilience learnt during service.
Using existing systems to support care
Lifestyle interventions are more sustainable when embedded within veteran-specific systems.
Veterans’ Health Check
- provides a structured entry point to identify lifestyle risks
- supports prioritisation using a veteran-centred lens
- facilitates early referral to appropriate services
- enables team-based care planning for veterans with multimorbidity or complex needs
- supports regular review and shared care between GPs, practice nurses, and allied health providers
- improves continuity and accountability for lifestyle-related goals
- delivers trauma-informed mental health, peer, and family support
- improves engagement in lifestyle change when post-traumatic stress disorder, grief, or transition stressors are present
Peer-based and group programs
- include veteran hubs, group Heart Health programs, and community activities
- strengthen social connection, identity, and routine
- reinforce behaviour change beyond the consulting room
References
- Australian Society of Lifestyle Medicine. Lifestyle Medicine Vital Signs. 2024. Available at: https://lifestylemedicine.org.au. (last accessed Feb 2026).
- Department of Veterans’ Affairs. Veteran health and wellbeing strategy. 2022. Available at: https://www.dva.gov.au. (last accessed Feb 2026).
- Egger, G., Binns, A., Rossner, S., & Sagner, M. Lifestyle medicine (3rd ed.). 2017. McGraw-Hill.
- Prochaska, J. O., & DiClemente, C. C. Stages and processes of self-change. Journal of Consulting and Clinical Psychology. 1983; 51(3):390–395.
- StatPearls. Transtheoretical model of change. 2023. National Centre for Biotechnology Information. Available at: https://www.ncbi.nlm.nih.gov/books/NBK556005/. (last accessed Feb 2026).
Claim your CPD
After reading the clinical summary above and reviewing the references, complete the quiz to gain 30 minutes of EA CPD and 30 minutes of RP CPD.
You can either self-report CPD to your CPD home, or Medcast will track your learning via your personal CPD Tracker and you can download and report these points once a year. See our CPD Tracker FAQ.
Quiz
Please log in or sign up for a free Medcast account to access the case study questions and achieve the CPD credits.

Dr Nazha Nazeem is a General Practitioner based in Melbourne, Victoria, with a dynamic footprint in medical education—especially supporting International Medical Graduates (IMGs) transitioning into Australian General Practice. After earning her MD from the University of Melbourne in 2018, she completed her Fellowship with the RACGP and is currently pursuing a Master’s in Lifestyle Medicine at James Cook University.
She is passionate about crafting learner-centred educational experiences that are practical, relevant, and supportive—ensuring education translates into real-life practice.
Become a member and get unlimited access to 100s of hours of premium education.
Learn moreAllied health professionals play a vital role in veteran care. This guide outlines DVA card types, the allied health treatment cycle, exceptions and billing essentials – introducing allied health providers to practical knowledge that enables delivery of compliant veteran-centred care under Department of Veterans' Affairs arrangements.
The General Practice in Aged Care Incentive scheme (GPACI) was designed to improve health outcomes for permanent residents of aged care homes. This FastTrack outlines the core requirements, including patient, GP, and practice eligibility, and how to take advantage of the program while maintaining compliance. 30mins each RP and EA available.
Minor procedures are part of a GP’s daily practice, yet MBS items are often not used correctly, risking non-compliance or missed revenue. This FastTrack provides a concise overview of common procedural item numbers in the MBS, including a refresher of key points to support billing compliance. 30mins each RP and EA available.
